In a game called Last Man Standing, about 31 adults stood around a plastic folding table outside the community centre. Each person had one hand on the table, where they had to keep it or be eliminated. The last one remaining, a man who stood for 16.5 hours without lifting his hand, walked away with keys to a new all-terrain vehicle.
It was one of many activities at Neskantaga’s spring carnival, an annual week-long celebration the remote community in Northern Ontario could hold because it created a bubble with stringent pandemic protocols, and at least 89 per cent of the eligible population have received both doses of the Moderna COVID-19 vaccine.
Neskantaga is among 31 communities that participated in Operation Remote Immunity, a vaccination program led by Ontario’s Ornge air ambulance service in collaboration with Nishnawbe Aski Nation, a political territorial organization representing 49 mostly remote First Nations in Northern Ontario.
Homer Tien, president and chief executive officer of Ornge, was appointed head of the province’s vaccine task force recently, after retired general Rick Hillier stepped down when his contract expired at the end of March.
Dr. Tien said the success of the program, which winds down this week, is a result of the strong and respectful partnership with First Nations leaders in developing a plan that addressed their needs.
Ornge spokesperson Joshua McNamara said about 25,000 doses have been administered, including more than 14,000 first doses and more than 10,000 second doses, since the program launched in late January. He would not give the uptake rates for each community.
Dr. Tien said each community produced its own list of eligible adults, taking into account variables such as the fact that not all registered band members live on-reserve. He said as a result, the communities report higher uptake rates than Ornge’s records do, but that he will include both sets of data in his reporting.
In November, when the Canadian government was close to approving a COVID-19 vaccine, First Nations chiefs in Northern Ontario were gearing up to get vaccinations to the remote north, where historic and current government policies have left housing and health outcomes for Indigenous people in such a grim state that COVID-19 would be devastating.
The National Advisory Committee on Immunization (NACI) identified Indigenous communities as a priority because congregate living and working conditions put them at an elevated risk of infection with disproportionate consequences.
Given the logistical challenges in the remote north, including getting to communities by plane in winter, when minus-40 temperatures and other weather conditions determine whether an aircraft can land, it was imperative to have a plan that worked for them.
Lynne Innes, president and chief executive officer of Weeneebayko Area Health Authority (WAHA) in Moose Factory, which provides public health care to six communities along the James Bay and Hudson Bay coasts, said uptake ranges from 70 to 94 per cent, with a goal of reaching 95 per cent.
Ms. Innes, who was co-lead of the rollout for her region, attributes their success to developing distribution models based on each community’s needs. These included building trust, something easily established by having their own human health resources, such as nurses, paramedics and elders, work with the vaccinators from Ornge, she said. Any vaccine hesitancy was addressed through public health campaigns on social media and local radio in the Cree dialects, and personal community visits from Ms. Innes, who is a Cree from Moose Factory, and an elder.
Dr. Tien said the Ornge vaccination teams consisted of a paramedic lead and other paramedics, nurses and physicians recruited from universities and emergency services.
Lisa Richardson, an Anishinaabe internal medicine physician at the University of Toronto, was one of the vaccinators that went to Sandy Lake in March. On a chartered plane, the Ornge team strapped the small freezer box of vaccine doses into its own seat as they flew in and out of the community each day for a scheduled 10 days. Weather cancelled a few of those.
Dr. Richardson said Ornge and the First Nations leaders had an understanding that the vaccination clinics would be guided by each community’s requirements, and that it was clear Ornge’s role was to provide medical, technical and logistical expertise. The communities practiced in advance, and had the clinics set up and ready.
“All that we had to do was to go in and be the expert vaccinators,” Dr. Richardson said. “And obviously, be respectful and have fun.”
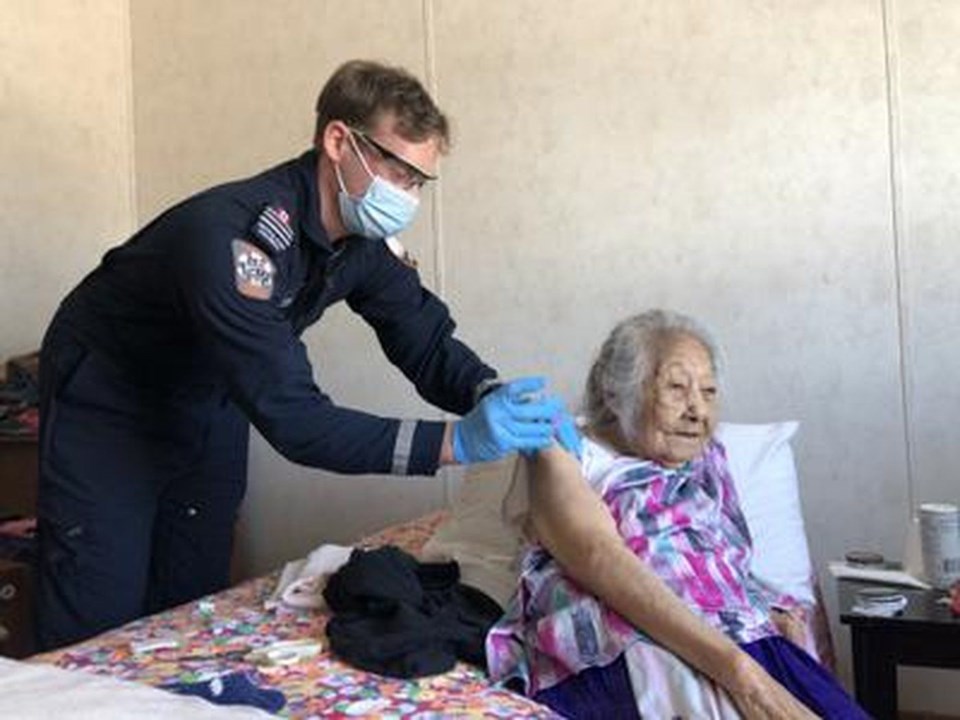
Vaccinators went to the homes of those who couldn’t attend the clinics, sitting and visiting during the 15-minute observation period afterwards.
Pandemic restrictions in many of the remote communities have been tight, and remain so because risks remain for children and others not vaccinated. Travel is only allowed for essential reasons, like medical appointments and family emergencies, and hot spots such as Thunder Bay and Winnipeg are off limits. People are required to isolate and get tested when they return.
Ms. Innes said as Operation Remote Immunity winds down, the communities are transitioning to a program that will ensure that everyone who got the first dose gets the second one, and will continue vaccinating people until they get to at least 95 per cent.
She said reaching the target will give more freedom to travel among the six communities, which is important to people in the family-based Cree culture, who are looking forward to going to their camps for spring geese hunting.
Between January and March, Indigenous Services reported more than 12,000 confirmed cases of COVID-19 in First Nations across the country, and just over 2,300 since March.
At a news conference on Wednesday, Marc Miller, Minister of Indigenous Services, said infection rates in First Nations are dropping as a result of vaccinations in more than 600 communities, with more than 264,000 doses administered as of this week.
Willow Fiddler is a Local Journalism Initiative (LJI) reporter with The Globe and Mail. The LJI program is funded by the Government of Canada.